 Sanjeeva Srivastava, Ph.D.
Sanjeeva Srivastava, Ph.D.
Assistant Professor, Proteomics Lab, IIT-Bombay, India
Identification of Potential Early Diagnostic Biomarkers for Gliomas and Various Infectious Diseases using Proteomic Technologies
The spectacular advancements achieved in the field of proteomics research during the last decade have propelled the growth of proteomics for clinical research. Recently, comprehensive proteomic analyses of different biological samples such as serum or plasma, tissue, CSF, urine, saliva etc. have attracted considerable attention for the identification of protein biomarkers as early detection surrogates for diseases (Ray et al., 2011). Biomarkers are biomolecules that can be used for early disease detection, differentiation between closely related diseases with similar clinical manifestations as well as aid in scrutinizing disease progression. Our research group is performing in-depth analysis of alteration in human proteome in different types of brain tumors and various pathogenic infections to obtain mechanistic insight about the disease pathogenesis and host immune responses, and identification of surrogate protein markers for these fatal human diseases.
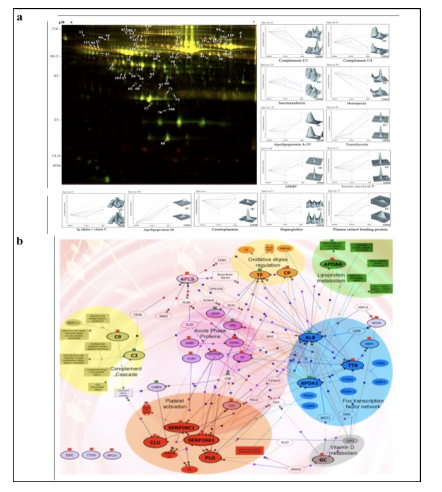
Applying 2D-DIGE in combination with MALDI-TOF/TOF MS we have analyzed the serum and tissue proteome profiles of glioblastoma multiforme; the most common and lethal adult malignant brain tumor (Gollapalli et al., 2012) (Figure 1). Results obtained were validated by employing different immunoassay-based approaches. In serum proteomic analysis we have identified some interesting proteins like haptoglobin, ceruloplasmin, vitamin-D binding protein etc. Moreover, proteomic analysis of different grades (grade-I to IV) of gliomas and normal brain tissue was performed and differential expressions of quite a few proteins such as SIRT2, GFAP, SOD, CDC42 have been identified, which have significant correlation with the tumor growth. While proteomic analysis of cerebrospinal fluid from low grade (grade I & II) vs. high grade (grade III & IV) gliomas revealed modulation of CSF levels of apolipoprotein E, dickkopf related protein 3, vitamin D binding protein and albumin in high grade gliomas. The prospective candidates identified in our studies provide a mechanistic insight of glioma pathogenesis and identification of potential biomarkers. We are also studying the role of JAK/STAT interactome and therapeutic potential of STAT3 inhibitors in gliomas using proteomics approach. Several candidates of the JAK/STAT interactome were identified with altered expression and a significant correlation was observed between STAT3 and PDK1 transcript expression level.
We have also investigated the changes in human serum proteome in different infectious diseases including falciparum and vivax malaria (Ray et al., 2012a; Ray et al., 2012b), dengue (Ray et al., 2012c) and leptospirosis (Srivastava et al., 2012). Although, quite a few serum proteins were found to be commonly altered in different infectious diseases and might be a consequence of inflammation mediated acute phase response signaling, uniquely modulated candidates were identified in each pathogenic infection indicating the some inimitable responses. Further, a panel of identified proteins consists of six candidates; serum amyloid A, hemopexin, apolipoprotein E, haptoglobin, retinol-binding protein and apolipoprotein A-I was used to build statistical sample class prediction models employing PLSDA and other classification methods to predict the clinical phenotypic classes and 91.37% overall prediction accuracy was achieved (Figure 2). ROC curve analysis was carried out to evaluate the individual performance of classifier proteins. The excellent discrimination among the different disease groups on the basis of differentially expressed proteins demonstrates the potential diagnostic implications of this analytical approach.
Keywords: Diagnostic biomarkers, Gliomas, Infectious Diseases, Proteomics, Serum proteome
Acknowledgments: This disease biomarker discovery research was supported by Department of Biotechnology, India grant (No. BT/PR14359/MED/30/916/2010), Board of Research in Nuclear Sciences (BRNS) DAE young scientist award (2009/20/37/4/BRNS) and a startup grant 09IRCC007 from the IIT Bombay. The active support from Advanced Center for Treatment Research and Education in Cancer (ACTREC), Tata Memorial Hospital (TMH), and Seth GS Medical College and KEM Hospital Mumbai, India in clinical sample collection process is gratefully acknowledged.
References :
- Ray S, Reddy PJ, Jain R, Gollapalli K. Moiyadi A, Srivastava S. Proteomic technologies for the identification of disease biomarkers in serum: advances and challenges ahead. Proteomics 11: 2139-61, 2011.
- Gollapalli K, Ray S, Srivastava R, Renu D, Singh P, Dhali S, Dikshit JB, Srikanth R, Moiyadi A, Srivastava S. Investigation of serum proteome alterations in human glioblastoma multiforme. Proteomics 12(14): 2378-90, 2012.
- Ray S, Renu D, Srivastava R, Gollapalli K, Taur S, Jhaveri T, Dhali S, Chennareddy S, Potla A, Dikshit JB, Srikanth R, Gogtay N, Thatte U, Patankar S, Srivastava S. Proteomic investigation of falciparum and vivax malaria for identification of surrogate protein markers. PLoS One 7(8): e41751, 2012a.
- Ray S, Kamath KS, Srivastava R, Raghu D, Gollapalli K, Jain R, Gupta SV, Ray S, Taur S, Dhali S, Gogtay N, Thatte U, Srikanth R, Patankar S, Srivastava S. Serum proteome analysis of vivax malaria: An insight into the disease pathogenesis and host immune response. J Proteomics 75(10): 3063-80, 2012b.
- Srivastava R, Ray S, Vaibhav V, Gollapalli K, Jhaveri T, Taur S, Dhali S, Gogtay N, Thatte U, Srikanth R, Srivastava S. Serum profiling of leptospirosis patients to investigate proteomic alterations. J Proteomics 76: 56-68, 2012.
- Ray S, Srivastava R, Tripathi K, Vaibhav V, Srivastava S. Serum proteome changes in dengue virus-infected patients from a dengue-endemic area of India: towards new molecular targets? OMICS 16(10): 527-36, 2012c.
* Correspondence: Dr. Sanjeeva Srivastava, Department of Biosciences and Bioengineering, IIT Bombay, Mumbai 400 076, India: E-mail: sanjeeva@iitb.ac.in; Phone: +91-22-2576-7779, Fax: +91-22-2572-3480
![Figure 2 (a) Western blot analysis of haptoglobin (HP), serum amyloid A (SAA), and clusterin (CLU) from serum samples of healthy control (HC) [n = 12], falciparum malaria (FM) [n = 12], vivax malaria (VM) [n = 12], Leptospirosis (Lep) [n = 6], dengue fever [DF] [n = 6] and non infectious disease control (NIDC:GBM) [n = 12]. Representative blots of the target proteins are depicted along with their respective relative abundance volumes (volume X 104). All the data are represented as mean ± SE. (b) Discrimination of malaria from dengue, leptospirosis and GBM using PLS-DA analysis. PLS-DA scores Plot for FM (blue spheres, n = 8), VM (green spheres, n = 8), DF (red spheres, n = 6), Lep (grey spheres, n = 6) and GBM (brown spheres, n = 8) samples based on 6 differentially expressed proteins (serum amyloid A, hemopexin, apolipoprotein E, haptoglobin, retinol-binding protein and apolipoprotein A-I) identified using DIGE. The axes of the plot indicate PLSDA latent variables t0-t2.](http://www.amritabioquest.org/conference/2013/wp-content/uploads/sites/2/2015/02/sanjeeva-2.jpg)
 Nader Pourmand, Ph.D.
Nader Pourmand, Ph.D.
Director, UCSC Genome Technology Center,University of California, Santa Cruz
Biosensor and Single Cell Manipulation using Nanopipettes
Approaching sub-cellular biological problems from an engineering perspective begs for the incorporation of electronic readouts. With their high sensitivity and low invasiveness, nanotechnology-based tools hold great promise for biochemical sensing and single-cell manipulation. During my talk I will discuss the incorporation of electrical measurements into nanopipette technology and present results showing the rapid and reversible response of these subcellular sensors to different analytes such as antigens, ions and carbohydrates. In addition, I will present the development of a single-cell manipulation platform that uses a nanopipette in a scanning ion-conductive microscopy technique. We use this newly developed technology to position the nanopipette with nanoscale precision, and to inject and/or aspirate a minute amount of material to and from individual cells or organelle without comprising cell viability. Furthermore, if time permits, I will show our strategy for a new, single-cell DNA/ RNA sequencing technology that will potentially use nanopipette technology to analyze the minute amount of aspirated cellular material.
 R. Manjunath, Ph.D.
R. Manjunath, Ph.D.
Associate Professor, Dept of Biochemistry, Indian Institute of Science, Bengaluru, India
REGULATION OF THE MHC COMPLEX AND HLA SOLUBILISATION BY THE FLAVIVIRUS, JAPANESE ENCEPHALITIS VIRUS
Viral encephalitis caused by Japanese encephalitis virus (JEV) and West Nile Virus (WNV) is a mosquito-borne disease that is prevalent in different parts of India and other parts of South East Asia. JEV is a positive single stranded RNA virus that belongs to the Flavivirus genus of the family Flaviviridae. The genome of JEV is about 11 kb long and codes for a polyprotein which is cleaved by both host and viral encoded proteases to form 3 structural and 7 non-structural proteins. It is a neurotropic virus which infects the central nervous system (CNS) and causes death predominantly in newborn children and young adults. JEV follows a zoonotic life-cycle involving mosquitoes and vertebrate, chiefly pigs and ardeid birds, as amplifying hosts. Humans are infected when bitten by an infected mosquito and are dead end hosts. Its structural, pathological, immunological and epidemiological aspects have been well studied. After entry into the host following a mosquito bite, JEV infection leads to acute peripheral neutrophil leucocytosis in the brain and leads to elevated levels of type I interferon, macrophage-derived chemotactic factor, RANTES,TNF-α and IL-8 in the serum and cerebrospinal fluid.
Major Histocompatibility Complex (MHC) molecules play a very important role in adaptive immune responses. Along with various classical MHC class I molecules, other non-classical MHC class I molecules play an important role in modulating innate immune responses. Our lab has shown the activation of cytotoxic T-cells (CTLs) during JEV infection and CTLs recognize non-self peptides presented on MHC molecules and provide protection by eliminating infected cells. However, along with proinflammatory cytokines such as TNFα, they may also cause immunopathology within the JEV infected brain. Both JEV and WNV, another related flavivirus have been shown to increase MHC class I expression. Infection of human foreskin fibroblast cells (HFF) by WNV results in upregulation of HLA expression. Data from our lab has also shown that JEV infection upregulates classical as well as nonclassical (class Ib) MHC antigen expression on the surface of primary mouse brain astrocytes and mouse embryonic fibroblasts.
There are no reports that have discussed the expression of these molecules on other cells like endothelial and astrocyte that play an important role in viral invasion in humans. We have studied the expression of human classical class I molecules HLA-A, -B, -C and the non-classical HLA molecules, HLA-E as well as HLA-F in immortalized human brain microvascular endothelial cells (HBMEC), human endothelial cell line (ECV304), human glioblastoma cell line (U87MG) and human foreskin fibroblast cells (HFF). Nonclassical MHC molecules such as mouse Qa-1b and its human homologue, HLA-E have been shown to be the ligand for the inhibitory NK receptor, NKG2A/CD94 and may bridge innate and adaptive immune responses. We show that JEV infection of HBMEC and ECV 304 cells upregulates the expression of HLA-A, and –B antigens as well as HLA-E and HLA-F. Increased expression of total HLA-E upon JEV infection was also observed in other human cell lines as well like, human amniotic epithelial cells, AV-3, FL and WISH cells. Further, we show for the first time that soluble HLA-E (sHLA-E) was released from infected ECV and HBMECs. In contrast, HFF cells showed only upregulation of cell-surface HLA-E expression while U87MG, a human glioblastoma cell line neither showed any cell-surface induction nor its solubilization. This shedding of sHLA-E was found to be dependent on matrix metalloproteinase (MMP) and an important MMP, MMP-9 was upregulated during JEV infection. Treatment with IFNγ resulted in the shedding of sHLA-E from ECV as well as U87MG but not from HFF cells. Also, sHLA-E was shed upon treatment with IFNβ and both IFNβ and TNFα, when present together caused an additive increase in the shedding of sHLA-E. HLA-E is an inhibitory ligand for CD94/NKG2A receptor of Natural Killer cells. Thus, MMP mediated solubilization of HLA-E from infected endothelial cells may have important implications in JEV pathogenesis including its ability to compromise the blood brain barrier.



